How common are strokes?
Strokes are the third most frequent cause of death after heart diseases and cancer.
How are strokes classified?
Strokes are classified into ischemic and hemorrhagic. Eighty percent of strokes are ischemic and 20% hemorrhagic. Hemorrhagic strokes are further classified into intracerebral hematomas and subarachnoid hemorrhage.
What are the most common causes of strokes?
The most common causes of strokes are arteriosclerosis, embolic heart diseases, jugular vein dilatation, and vascular dysplasia (aneurysms and arteriovenous malformations). Risk factors for a stroke are old age, arterial hypertension, diabetes, atrial fibrillation, smoking, alcoholism, family history, obesity, lack of exercise, and dyslipidemia (high cholesterol and/or high triglycerides).
What is the clinical picture of strokes?
The clinical picture of strokes is defined by the sudden appearance of neurological symptoms that can include limb mobility disorders (hemiparesis or hemiplegia), sense perception disorders (hypesthesia), vision disorders (diplopy-temporary loss of visionhemianopsia), speech disorders (dysphasia, aphasia), headache, vertigo, and consciousness disorders (from lethargy to coma).
How is the classification of strokes done?
The CT scan is the visual representation of the brain that will classify whether a stroke is ischemic or hemorrhagic. Most of the time, the CT scan is performed before the patient’s admission to the hospital and is the deciding factor regarding the department that the patient will be admitted to. Severe stroke patients are initially admitted to an Intensive Care Unit (ICU). Less severe ischemic stroke patients are admitted to Pathology departments while hemorrhagic stroke patients are admitted to Neurosurgery departments since it is likely they will need an operation.
What is an ischemic stroke?
Ischemic strokes occur when the arteries to the brain are narrowed or blocked for any reason, causing severely reduced blood flow in a part of the brain, just like it happens during an acute heart attack. Nerve cells only survive for a few minutes after an ischemic episode; therefore, permanent and irreversible damage occurs in the specific part of the brain. This means that the nerve cells lost due to such an episode will never be replaced.
What is the clinical picture of ischemic strokes?
In the case of a full recovery within 24 hours from the symptoms’ appearance, the ischemic stroke is classified as transient. In the case of a full recovery within 7 days, the stroke is classified as reversible. In the case the patient has a permanent disability, then the stroke is classified as permanent. Transient and reversible ischemic strokes should be assessed thoroughly by a neurologist because the quick treatment will prevent a permanent stroke, and therefore a permanent disability. Further necessary diagnostic checks in these cases include a carotid and spinal arteries ultrasound as well as a thorough cardiac examination. In the case of a carotid stenosis over 70%, a vascular surgeon needs to examine the patient in order to decide the way of treatment (angioplasty with balloon or carotid endarterectomy).
What is a hemorrhagic stroke?
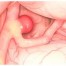
Hemorrhagic strokes occur when there is a brain vessel rupture and an intracranial hematoma is formed. This hematoma is a collection of blood within the brain parenchyma or a subarachnoid hemorrhage, that is a blood leak in the cerebrospinal fluid surrounding the brain. The severity of such a stroke is defined by a large degree on the amount of blood that leaks into the brain.
Subarachnoid hemorrhage in CT scan
What are the most common causes of hemorrhagic strokes?
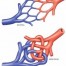
The most common reasons of a hemorrhagic stroke are a brain aneurysm rupture or an arteriovenous malformation. An aneurysm is like a balloon on a vessel wall, usually where it branches, and this happens because of a congenital fault in the structure of the vessel in combination with the constant pressure that it gets by the blood flow, especially if the arterial pressure is high (hypertension). An arteriovenous (AVM) malformation is a collection of poorly formed brain vessels that doesn’t include any brain parenchyma or capillary vessels, but only arteries and veins. It is of congenital etiology and it can be manifested either as an epileptic seizure or as a hemorrhagic stroke.
What is the cause of the aneurysm creation?
The exact cause of the aneurysm creation is unknown. However, aneurysms have
been observed in various pathological conditions, such as:
• hypertension
• fibromuscular dysplasia
• Ehlers-Danlos syndrome type IV (congenital collagen disorder)
• Marfan syndrome
• polycystic kidney disease
• lupus
• aortic isthmus stenosis
• familial intracranial aneurysm syndrome
How common is the brain aneurysm creation and how often does it rupture?
It is estimated that about 3% of the population has a brain aneurysm. Of this population, many have more than one aneurysm in various points and of various sizes. However, only half of them will rupture at some point of the patients’ life.
What is the clinical picture of a brain aneurysm rupture?
The brain aneurysm rupture causes subarachnoid hemorrhage that is clinically manifested with an extremely strong headache, vomiting, a stiff neck and neck pain, photophobia, consciousness loss, coma, and neurological symptoms, such as hemiparesis, aphasia, and so on.
Do brain aneurysms show any signs before they rupture?
Aneurysms show some warning signs before they rupture but patients usually ignore them. Minor hemorrhage, up to ten days prior the big rupture, may cause warning headaches. Headaches may also be caused without hemorrhage because of thrombosis, hemorrhagic dilation, or intramural hemorrhage. These headaches are described as acute and very strong, resembling a thunder. One-sided, retrobulbar headaches lasting more than 15 days can be caused by an irritation of the neighboring dura mater due to a touching aneurysm. Temporary blindness in one eye or hemianopsia may appear up to 21 days prior the aneurysm rupture.
Other symptoms of an intracranial aneurysm include:
• epileptic seizure
• hemiparesis caused by the pressure of a giant aneurysm
• paresis of the motor nerve with internal and external ophthalmoplegia (ptosis, diplopia)
• Reduction of vision because of optic nerve compression caused by an aneurysm in
the ophthalmic artery
• trigeminal neuralgia caused by an aneurysm in the cavernous sinus
• endocrine disorders caused by the compression of the hypophyseal branch by an
aneurysm
The aforementioned symptoms impose the imaging scan of the brain as well as the clinical examination by a neurosurgeon in order to locate an aneurysm as quickly as possible along with its likely rupture. Finally, numerous cases of aneurysms with no apparent symptoms are found randomly during a CT or an MRI brain scan that is performed for a different reason.
Headache may be caused a few days or weeks prior the aneurysm rupture.
How is a stroke treated at the Emergency Room of a hospital?
The correct treatment of strokes at the ER ensures a higher percentage of the patient’s
survival and decreases the likelihood of a residual disability. The emergency
treatment practice for a stroke is:
a) Ensuring that airways are accessible, even with intubation in case the patient is in a coma.
b) Oxygen administration with the help of a nasal catheter or a Venturi mask in case the patient is not intubated.
c) Intravenous administration of saline.
d) Blood pressure stabilization (systolic: 160–180 mmHg and diastolic: 90–100 mmHg) Hypertension in ischemic strokes is treated pharmaceutically only in the case of the systolic pressure being over 220 mmHg or the diastolic over 120 mmHg.
e) Nasogastric catheter (Levin) placement.
f) CT scan of the brain.
What is the special treatment of ischemic strokes?
Most of the ischemic strokes can be treated with a quick (within the first 6 hours) intravenous administration of thrombolytic and antithrombotic medication. With this treatment, clots are dissolved and blood circulation in the ischemic area of the brain is restored. This treatment should always be administered while closely monitoring the
patient with immediate access to a neurosurgeon as there is a high risk of causing an iatrogenic hemorrhagic stroke.
What is the special treatment of hemorrhagic strokes?
Hemorrhagic strokes are divided into intracranial hematomas and subarachnoid hemorrhages. Intracranial hematomas, depending on their position and size, may be treated conservatively until they are completely absorbed. However, their surgical removal may be deemed necessary either through a craniotomy or trepanation and stereotactic aspiration in order to ensure the patient’s survival. Intravenous administration of vasodepressor agents is required for the subarachnoid hemorrhage in order to prevent the vasospasm caused by it. In every hemorrhagic stroke, an angiography is required (digital subtraction angiography or noninvasively by three-dimensional angiography or MRA), that is the imaging of the vessels in order to accurately determine the damage caused by the hemorrhage as well as its position after the stabilization of the patient’s clinical condition.
The best type of angiography is the digital subtraction angiography, even though it is the most invasive and painful one because it allows both diagnostic and treatment procedures depending on the findings. If an aneurysm is the cause of a hemorrhagic stroke, it can be treated with embolization, that is special coils are placed in the sac that helps block the flow of blood into the aneurysm. If, however, embolization of the aneurysm is not possible, surgical clipping (with craniotomy) must be performed with aneurysm clips to prevent blood flow into the aneurysm. This method is performed with the assistance of a microscope and special microtools. Embolization is also successfully performed when the cause of the hemorrhage is an arteriovenous malformation.
How can we prevent a stroke?
The risk of a stroke can be decreased if the below mentioned tips are followed:
- Regular check of blood pressure
- Quit smoking
- Minimize alcohol consumption
- Extra weight loss
- Regular exercise
- Regular check of diabetes and blood lipids
- Cardiac check and treatment of arrhythmia along with possible administration
of antiplatelet drugs (Salospir, Plavix, Ticlid, etc.) - Check of arteries with a carotid and spinal arteries ultrasound